Sepsis, which used to be known as blood poisoning, arises when tissues and organs are damaged as a result of the body’s immune system overreacting to an infection, which quickly becomes life threatening.
Late diagnosis and antibiotic resistance are making it increasingly difficult to treat bacterial infections and to prevent them from developing into sepsis. Every year about 49 million people develop sepsis1, and one in five of them dies. Those who survive often suffer permanent damage.
Sepsis explained in 3 minutes
Source: World Sepsis Day – www.worldsepsisday.org.
The following symptoms might indicate sepsis:
- Slurred speech or confusion
- Extreme shivering or muscle pain, fever
- Passing no urine all day
- Severe breathlessness
- It feels like you’re going to die
- Skin mottled or discolored
Source: www.worldsepsisday.org/sepsis
Other symptoms that may be signs of sepsis:
- Low blood pressure
- Low urine production
- Stains / rash on the skin
The most common sources of sepsis
It is estimated that up to 50% of all cases of sepsis can be attributed to healthcare associated infections,2 where urinary tract infection is one of the most common sources of sepsis as well as pneumonia and catheter related bloodstream infection. Consequently, preventing healthcare associated infections is crucial for reducing the occurrence of sepsis.
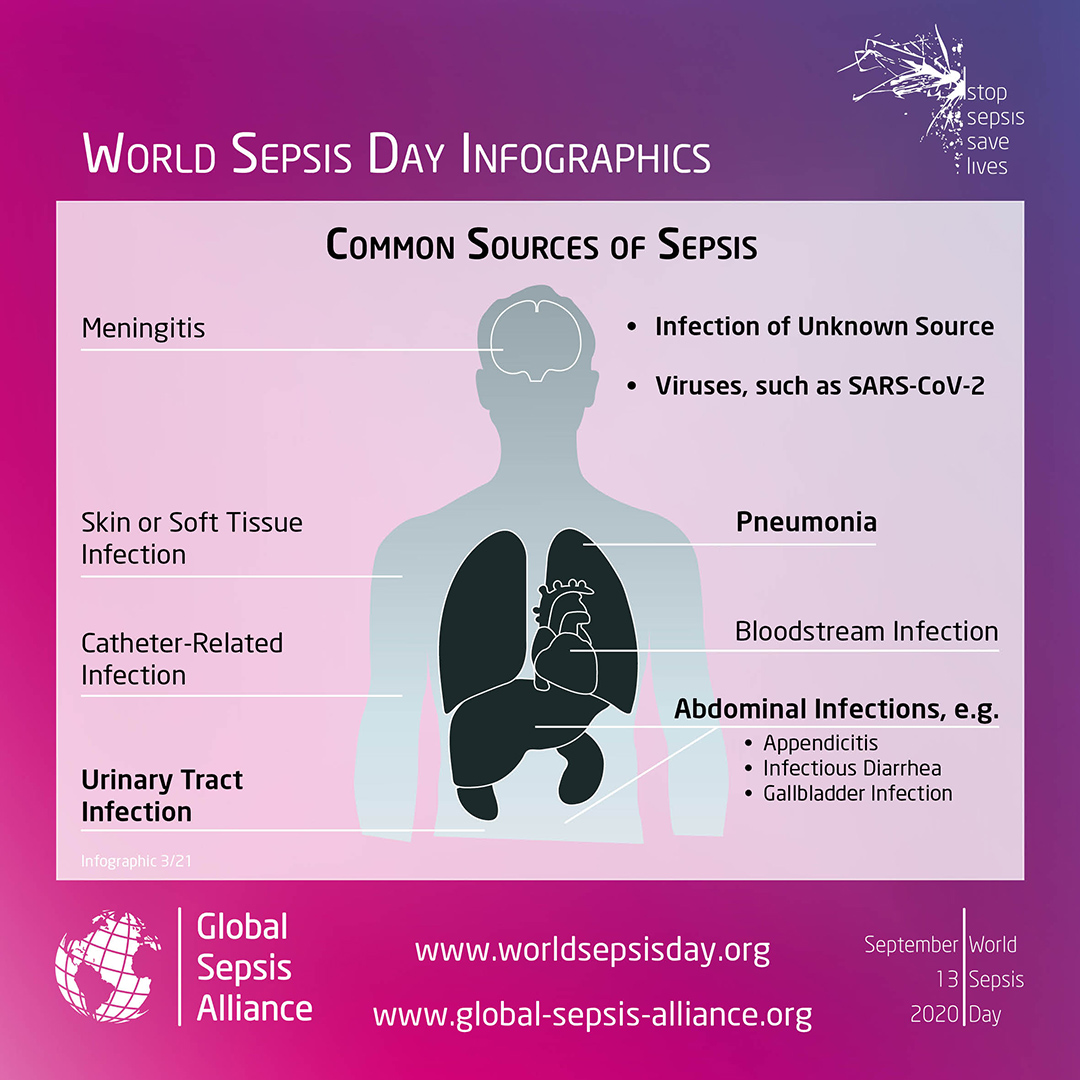

Source: World Sepsis Day – www.worldsepsisday.org. Click on the picture to enlarge.
Sepsis is a global health crisis
- 20% of all deaths worldwide are associated with sepsis
- Affects about 49 million people every year
- At least 11 million die – one death every 2.8 seconds
- Depending on country, mortality varies between 15 and more than 50 %
- Many surviving patients suffer from the consequences of sepsis for the rest of their lives
References:
1. Rudd, K. E (2020). Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. The Lancet, 395(10219), 200–211.
2. Eber MR et al. Arch Intern Med. 2010 Feb 22;170(4):347- 53. PMID:20177037.
